The syndrome of inappropriate antidiuresis (SIAD) refers to a group of clinical syndromes characterized by excessive secretion or enhanced effect of antidiuretic hormone (ADH, also known as arginine vasopressin), resulting in water retention, hyponatremia, and low plasma osmolality. Among these, the condition caused by excessive secretion of ADH is referred to as the syndrome of inappropriate secretion of antidiuretic hormone (SIADH) and is relatively common, representing the most frequent cause of hyponatremia. Enhanced ADH effect, however, leads to nephrogenic syndrome of inappropriate antidiuresis (NSIAD), which is rare. This section primarily focuses on SIADH.
Etiology and Pathophysiology
SIADH is commonly associated with malignancies, respiratory conditions, and central nervous system disorders. Idiopathic SIADH, with unknown causes, occurs more frequently in older individuals.
Ectopic AVP Secretion
Malignancies
Certain malignancies, such as small cell lung cancer, pancreatic cancer, lymphoma, duodenal cancer, and Hodgkin's lymphoma, can synthesize and release AVP, leading to SIADH. Among these, small cell lung cancer is the most common cause.
Pulmonary Infectious Diseases
Conditions like pneumonia, pulmonary tuberculosis, pulmonary abscess, and pulmonary aspergillosis may induce SIADH, potentially due to the synthesis and release of AVP by the affected pulmonary tissue.
Central Nervous System Disorders
Diseases such as brain trauma, brain abscess, brain tumor, subarachnoid hemorrhage, cerebral thrombosis, acute brain infections, tuberculous or other types of meningitis, and porphyria can disrupt hypothalamic-neurohypophyseal function, leading to excessive AVP secretion.
Medications
Certain drugs, including antidepressants (e.g., selective serotonin reuptake inhibitors), general anesthetics, barbiturates, carbamazepine, and chlorpropamide, can overstimulate AVP secretion and cause SIADH.
Excessive AVP release, which is not under normal regulatory mechanisms, increases water reabsorption in the distal tubules and collecting ducts. This prevents urine dilution and the excretion of free water, leading to extracellular fluid volume expansion, blood dilution, and reductions in both serum sodium concentration and plasma osmolality. Intracellular fluid also becomes hypotonic, causing cellular swelling. When brain cells are affected, neurological symptoms may arise. Despite extracellular fluid expansion, overall blood volume remains normal, and edema is typically absent. This occurs because the expanded extracellular volume suppresses proximal tubular sodium reabsorption, increasing urinary sodium excretion and preventing excessive water retention within the body. Additionally, extracellular volume expansion enhances the release of atrial natriuretic peptide, further promoting urinary sodium excretion. Sodium metabolism thus shifts toward a negative balance, exacerbating hyponatremia and low plasma osmolality. Furthermore, aldosterone secretion is inhibited, further increasing urinary sodium excretion.
Clinical Manifestations and Laboratory Findings
The primary features include water retention (dilutional hyponatremia), low plasma osmolality, and normal blood volume, typically without edema. The severity of symptoms depends on the degree of AVP secretion and the magnitude of water loading. Many patients do not exhibit classic symptoms under conditions of water restriction. However, if water intake exceeds the body's compensatory capacity, water retention and hyponatremia may become apparent. Serum sodium levels are generally below 130 mmol/L, while urinary sodium excretion remains relatively high (typically exceeding 20 mmol/L).
When serum sodium levels fall below 120 mmol/L, symptoms such as loss of appetite, nausea, vomiting, limb weakness, lethargy, and even confusion may occur. Serum sodium levels below 110 mmol/L may lead to muscle weakness, diminished or absent tendon reflexes, seizures, and coma, which, if untreated, can result in death. Plasma osmolality is often below 275 mOsm/(kg·H2O), while urine osmolality may exceed plasma osmolality. Despite adequate blood volume, the glomerular filtration rate increases, leading to reductions in blood urea nitrogen, creatinine, and uric acid concentrations. Plasma AVP levels remain inappropriately high relative to plasma osmolality.
Diagnosis and Differential Diagnosis
Diagnostic Criteria
The primary criteria for diagnosis include:
- Reduced serum sodium levels, often below 130 mmol/L.
- Increased urinary sodium levels, often exceeding 20 mmol/L or a daily urinary sodium excretion rate greater than 25 mmol.
- Reduced plasma osmolality, typically below 275 mOsm/(kg·H2O).
- Urine osmolality above 100 mOsm/(kg·H2O).
- Decreased levels of blood urea nitrogen, creatinine, and uric acid.
- Exclusion of other conditions, such as adrenal insufficiency, hypothyroidism, and the use of diuretics.
Etiological Diagnosis
Malignancies, particularly small cell lung cancer, are common causes. SIADH may precede the radiological changes of lung cancer. Central nervous system disorders, pulmonary infections, and medications should also be considered as potential causes.
Differential Diagnosis
Nephrogenic Syndrome of Inappropriate Antidiuresis (NSIAD)
This condition results from mutations in the V2R gene for AVP receptors in renal tubules (e.g., R137C, R137L) that activate the α subunit of the receptor's associated G protein, enhancing antidiuretic effects. It is an X-linked recessive disorder and exhibits reduced blood AVP levels. If hyponatremia occurs in children or multiple family members, or if the patient does not respond well to tolvaptan therapy, NSIAD should be considered, with further blood AVP and V2R gene testing as necessary. Drugs such as cyclophosphamide and sertraline can also activate AVP receptors in renal tubules, leading to hyponatremia, which may resolve after discontinuation of the offending medication.
Other Euvolemic Hyponatremias
Conditions such as adrenal insufficiency, nausea and emesis, and hypothyroidism are common causes of hyponatremia and require careful assessment of medical history and relevant tests for differentiation.
Hypovolemic Hyponatremia
This can result from gastrointestinal fluid losses (e.g., diarrhea), gastrointestinal, biliary, or pancreatic fistulae, or gastric decompression, wherein sodium loss exceeds water loss, leading to hyponatremia. A history of associated diseases and signs of dehydration is usually present. Blood urea nitrogen, creatinine, and uric acid levels tend to be elevated. Cerebral salt wasting syndrome (CSWS)—a condition in which intracranial disorders impair the kidney's ability to retain sodium, causing progressive sodium and water loss in the urine—leads to hyponatremia and extracellular fluid depletion. CSWS typically presents with hyponatremia, elevated urinary sodium levels, and hypovolemia. In contrast, SIADH is associated with normal blood volume. Additionally, CSWS responds to sodium and volume replacement therapy, whereas fluid restriction aggravates the condition instead of improving it.
Hypervolemic Hyponatremia
This occurs in cases of severe heart failure, cirrhosis, or nephrotic syndrome, where water retention exceeds sodium retention. Such patients generally exhibit a history of the underlying primary condition, along with symptoms like edema and ascites.
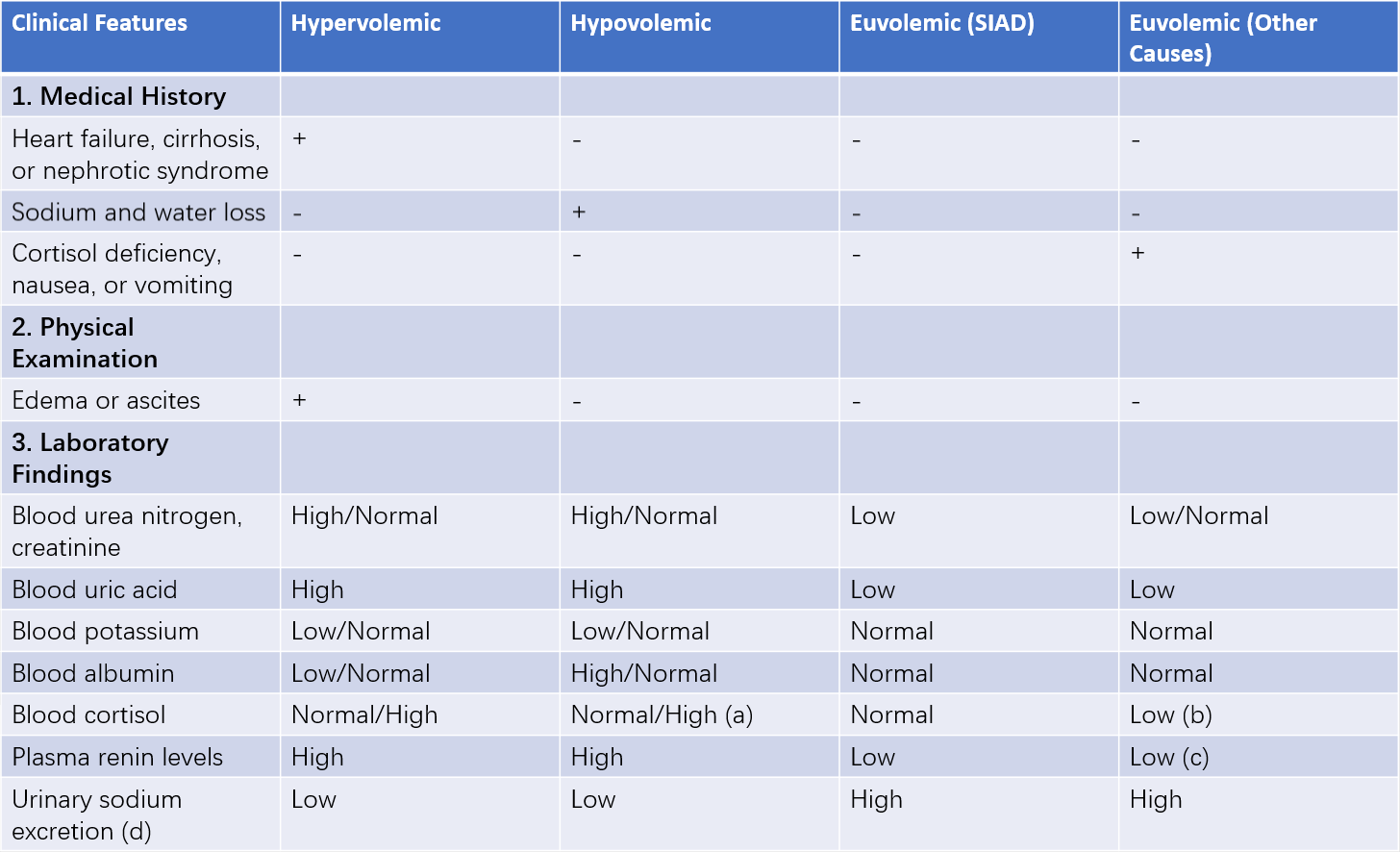
Table 1 Key points for differentiating hyponatremia based on extracellular fluid volume
Notes:
"+" indicates "present"; "-" indicates "absent."
a. In cases where hypovolemia is caused by primary adrenal insufficiency, blood cortisol levels are reduced.
b. In cases caused by nausea and emesis, blood cortisol levels may be normal or slightly elevated.
c. In cases of secondary adrenal insufficiency, plasma renin levels may be elevated.
d. Urinary sodium excretion rate is considered elevated in hyponatremia patients when >25 mmol/day.
Treatment
Etiological Treatment
Addressing the underlying condition is crucial. For cases induced by medications, discontinuing the offending drug is necessary.
Symptomatic Treatment
Water intake restriction is essential for symptom control. In mild cases, limiting daily water intake to 0.8–1.0 L typically alleviates symptoms, reduces body weight, and leads to increases in serum sodium levels and plasma osmolality. In severe cases, 20–40 mg of furosemide can be administered to facilitate water excretion. Severe hyponatremia (e.g., serum sodium levels below 110 mmol/L) may require intravenous infusions of 3% sodium chloride solution. The recommended infusion rate is 1–2 mL/(kg·h), allowing for a gradual rise in serum sodium while monitoring levels frequently (every 2–4 hours). It is crucial to avoid increasing serum sodium by more than 10–12 mmol/L within 24 hours. Once serum sodium levels reach approximately 120 mmol/L, hypertonic saline infusion can be discontinued. Excessively rapid corrections in serum sodium can lead to central pontine myelinolysis, which may present with symptoms such as dysarthria, mutism, dysphagia, lethargy, emotional changes, paralysis, seizures, coma, and even death.
Antidiuretic Hormone Receptor Antagonists
Tolvaptan selectively antagonizes V2R AVP receptors located in the basolateral membrane of renal collecting duct cells, reducing water permeability in these ducts and increasing water excretion, which raises serum sodium concentrations. The initial dosage is 15 mg once daily, with adjustment possible 24 hours after administration. Tolvaptan use does not necessitate water restriction, but serum electrolytes require monitoring to prevent overly rapid increases in serum sodium. Common side effects include dry mouth, thirst, dizziness, nausea, and hypotension.
Prognosis
The prognosis is poor in cases associated with malignancies such as small cell lung cancer and pancreatic cancer. For cases caused by non-malignant factors (e.g., pulmonary diseases, central nervous system disorders, hypothyroidism, or medications), SIADH typically resolves following effective treatment of the primary condition or discontinuation of the causative medication.