In clinical practice, disturbances of acid-base balance are almost always mixed disorders, and they change dynamically with the progression of the disease and the impact of therapeutic interventions.
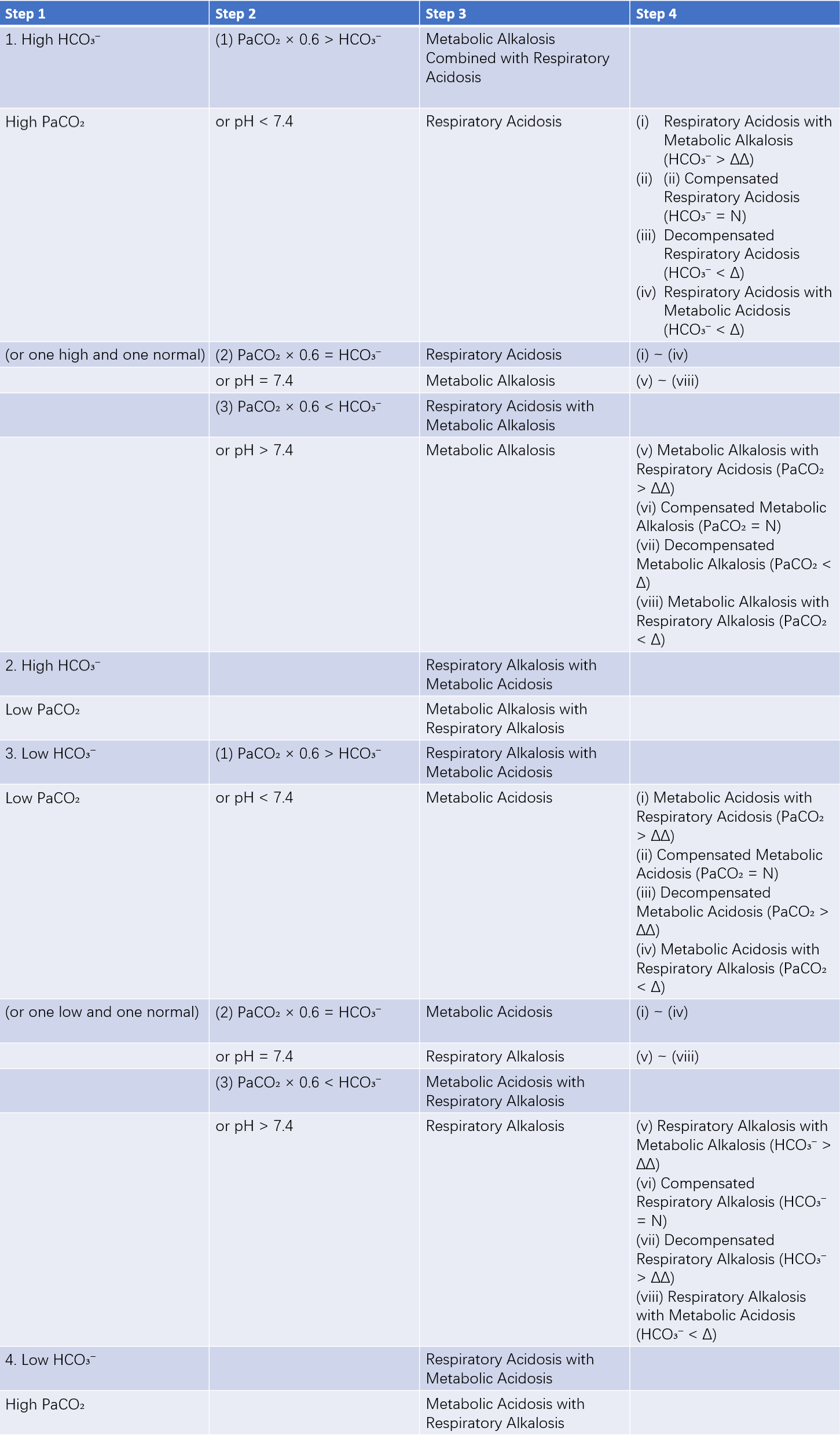
Table 1 Determination of acid-base imbalance types
Notes:
ΔΔ: Upper limit of expected compensatory range.
Δ: Lower limit of expected compensatory range.
N: Within the expected compensatory range.
Single-Factor Mixed Acid-Base Disorders
The underlying cause is either metabolic or respiratory in nature. Common combinations include:
Compensatory Mixed Acid-Base Disorders
These occur when secondary acid-base disturbances arise during the process of compensation:
- Metabolic Acidosis with Compensatory Respiratory Alkalosis: Primary reduction in HCO3- leads to a compensatory reduction in H2CO3, causing a decrease in blood pH (increase in H+ concentration).
- Metabolic Alkalosis with Compensatory Respiratory Acidosis: Primary increase in HCO3- leads to a compensatory increase in H2CO3, causing an increase in blood pH.
- Respiratory Acidosis with Compensatory Metabolic Alkalosis: Primary elevation of PaCO2 leads to a compensatory increase in HCO3-, causing a decrease in blood pH.
- Respiratory Alkalosis with Compensatory Metabolic Acidosis: Primary reduction in PaCO2 leads to a compensatory reduction in HCO3-, causing an increase in blood pH.
Exacerbated Mixed Acid-Base Disorders
These include:
- Mixed Metabolic Acidosis: For example, diabetic ketoacidosis combined with lactic acidosis.
- Mixed Metabolic Alkalosis: For example, hypokalemic alkalosis combined with hypochloremic alkalosis.
- Mixed Respiratory Acidosis: For example, chronic obstructive pulmonary emphysema combined with spinal deformities.
- Mixed Respiratory Alkalosis: For example, chest trauma combined with hyperventilation syndrome due to hysteria.
Offset Mixed Acid-Base Disorders
These include:
- Metabolic Acidosis with Metabolic Alkalosis: For example, diabetic ketoacidosis combined with hypokalemic alkalosis.
- Respiratory Acidosis with Respiratory Alkalosis: For example, severe pneumonia resulting in hypoventilation combined with hyperventilation due to high fever.
Double-Factor Mixed Acid-Base Disorders
These occur when both metabolic and respiratory factors simultaneously contribute to acid-base disturbances.
Exacerbated Mixed Acid-Base Disorders
These include:
- Metabolic Acidosis with Respiratory Acidosis: For example, diabetic ketoacidosis combined with severe pulmonary infection, leading to a marked decrease in blood pH, reduced HCO3- levels, and increased PaCO2.
- Metabolic Alkalosis with Respiratory Alkalosis: Blood pH increases significantly, with elevated HCO3- and reduced PaCO2 levels.
Offset Mixed Acid-Base Disorders
These include:
- Metabolic Acidosis with Respiratory Alkalosis: The two disturbances balance each other out, resulting in normal, elevated, or decreased blood pH, with reduced HCO3- and reduced PaCO2 levels.
- Metabolic Alkalosis with Respiratory Acidosis: These disturbances neutralize each other, resulting in normal, elevated, or decreased blood pH, with increased HCO3- and increased PaCO2 levels.
Triple Acid-Base Imbalances
When the anion gap (AG) exceeds 16 mmol/L, combined with medical history and clinical manifestations, it suggests the presence of metabolic acidosis. If the first three diagnostic steps indicate either respiratory acidosis + metabolic alkalosis or respiratory alkalosis + metabolic alkalosis, the final diagnosis may be triple acid-base imbalance of a respiratory acidosis type (metabolic acidosis + respiratory acidosis + metabolic alkalosis) or a respiratory alkalosis type (metabolic acidosis + respiratory alkalosis + metabolic alkalosis).