Behçet's disease (BD), also referred to as Behçet syndrome, is a chronic condition that primarily manifests with oral and genital ulcers, along with uveitis, and can involve multiple organ systems. It was first described in 1937 by Turkish professor Hulusi Behçet. The disease follows a relapsing-remitting course, alternating between flares and remission. While severe cases involving internal organ damage can lead to death, most individuals have a favorable prognosis. Behçet's disease demonstrates marked geographic variability, being more common in regions such as Mediterranean countries, China, Korea, and Japan. Incidence rates vary considerably, with the highest in Turkey (100–370 cases per 100,000 people) and the lowest in the United Kingdom (0.6 cases per 100,000 people). In northern China, the incidence is approximately 110 cases per 100,000 people. The condition is slightly more prevalent in men than women. Different subtypes of BD are identified based on organ system involvement, including vascular, neurological, and gastrointestinal types. Vascular BD involves large, medium, or small arteries and/or veins. Neurological BD is characterized by central or peripheral nervous system involvement. Gastrointestinal BD involves conditions like ulcers, hemorrhage, or perforation of the gastrointestinal tract.
Etiology
The exact cause remains unknown, but genetic predisposition and infections are believed to play a role.
Pathology
The fundamental pathological change in Behçet's disease is vasculitis. Infiltration of inflammatory cells into the vascular wall leads to thickened vessel walls and narrowed lumens, with severe cases showing vascular necrosis or aneurysm formation. Secondary thrombosis may also occur. Unlike other forms of vasculitis, Behçet's disease can affect large, medium, small, and microvessels, involving both arterial and venous vessels across a broad spectrum.
Clinical Manifestations
Core Symptoms
Oral Ulcers
Recurrent oral ulcers are the hallmark of Behçet's disease, occurring at least three times per year. Painful ulcers measuring 2–3 mm in diameter commonly appear on the buccal mucosa, tongue margins, lips, and soft palate. They typically resolve spontaneously within 7–14 days without leaving scars, although in some cases persistent ulcers lasting weeks may heal with scarring. Oral ulcers occur in over 98% of patients and are usually the first symptom to appear, making it the most essential and necessary diagnostic feature of the disease.
Genital Ulcers
Genital ulcers are present in approximately 80% of patients and share similar characteristics with oral ulcers. In women, they typically occur on the labia majora and minora and less commonly in the vagina. In men, ulcers are often found on the scrotum and penis but may also involve the perineum or areas around the anus.
Skin Lesions
Skin involvement in Behçet's disease can include erythema nodosum, acneiform rashes, and superficial thrombophlebitis. Erythema nodosum is the most common, affecting approximately 70% of patients. It typically appears symmetrically below the knees as erythematous, infiltrative, tender subcutaneous nodules that gradually enlarge. After 7–14 days, the nodules turn dark red, sometimes resolving spontaneously and leaving pigmentation without ulceration. Another type of skin manifestation is folliculitis, which may present with or without pustules, usually on the face and neck, and is observed in about 30% of patients. Skin hypersensitivity, such as local redness, swelling, or purulent reactions following needle puncture or minor trauma, represents a relatively specific cutaneous response in Behçet's disease. Superficial thrombophlebitis often involves the lower limbs and is characterized by linear redness, swelling, and tenderness along the vein during the acute phase. This may evolve into palpable, cord-like, thrombosed veins post-acute phase.
Ocular Involvement
The most frequent eye manifestations include uveitis and retinal vasculitis-induced retinitis. Recurrent eye inflammation may result in visual impairment or even blindness. Anterior uveitis (iridocyclitis), with or without hypopyon, causes relatively mild effects on vision. Retinitis due to retinal vasculitis may lead to optic nerve atrophy and significant vision loss.
Systemic Symptoms
In addition to the core symptoms, some patients experience visceral involvement caused by vasculitis, which typically occurs following the onset of the primary symptoms. Some individuals may also present with fever, fatigue, and weight loss during disease activity.
Gastrointestinal Involvement
This is also referred to as intestinal Behçet's disease and often occurs in patients with active disease. The most common symptom is abdominal pain, typically localized to the lower right quadrant and accompanied by tenderness and rebound pain. Additional symptoms include nausea, vomiting, bloating, loss of appetite, diarrhea, and difficulty swallowing.
The fundamental gastrointestinal lesion is characterized by multiple ulcers, which can occur anywhere from the esophagus to the descending colon, with a prevalence of up to 50%. Severe cases may develop complications such as ulcer bleeding, intestinal obstruction, intestinal perforation, peritonitis, fistula formation, or esophageal strictures, which can be life-threatening.
Nervous System Involvement
Also called neuro-Behçet's disease, it occurs in 20% of patients, typically manifesting within months to years after the appearance of core symptoms. Any part of the brain or spinal cord can be affected by small-vessel vasculitis, and clinical manifestations vary depending on the site of involvement. Onset is often acute, and symptoms can be classified into meningitis/meningoencephalitis, brainstem lesions, benign intracranial hypertension, spinal cord involvement, or peripheral nervous system impairment. Central nervous system venous thrombosis is also common, with patients experiencing severe headaches.
Cardiovascular System Involvement
Vascular lesions in Behçet's disease involve large and medium vessels and are observed in 10% of patients, referred to as vascular Behçet's disease.
Large and Medium Arteritis
Arterial involvement can occur in either systemic or pulmonary circulation, leading to stenosis and aneurysm formation, sometimes alternating segmentally within the same vessel. Large arteries are more commonly affected than medium-sized arteries.
Large and Medium Vein Inflammation
Venous involvement is characterized by significant thrombosis in addition to vascular wall inflammation. Large venous thrombophlebitis often results in narrowing or obstruction of the superior or inferior vena cava, leading to edema in distal tissues and corresponding symptoms. Thrombophlebitis in medium-sized veins is more commonly seen in the extremities, especially the lower limbs, and may also occur in cerebral veins.
Cardiac Complications
Cardiac involvement is less common but may include aortic regurgitation, mitral stenosis, mitral regurgitation, atrioventricular conduction block, myocardial infarction, and pericardial effusion.
Arthritis
Arthralgia affects 30%–50% of patients, presenting as pain, swelling, or limited mobility in one or a few joints. The knee joint is most commonly affected. Most episodes are transient, self-limiting, and can recur.
Lungs
Pulmonary arteritis involves inflammation of small pulmonary arteries, resulting in pulmonary aneurysm formation or local vascular thrombosis. Symptoms include hemoptysis, chest pain, and shortness of breath. Large-volume hemoptysis can be fatal. Patients with pulmonary embolism typically have a poor prognosis.
Epididymitis
Epididymitis can affect one or both sides, presenting as epididymal swelling, pain, and tenderness.
Laboratory Tests
No specific serum test exists for Behçet's disease. During the acute phase or active disease, findings may include anemia, elevated leukocyte and platelet counts, increased erythrocyte sedimentation rate (ESR), and elevated C-reactive protein (CRP). However, antibody markers such as ANAs, ANCA, and antiphospholipid antibodies are typically unremarkable. Complement levels and circulating immune complexes are usually normal, with occasional mild increases in globulin levels.
Positive Pathergy Test
The pathergy test is the only relatively specific test currently available for Behçet's disease. After disinfecting the skin, a sterile needle is used to puncture the dermis of the forearm, and the site is observed 48 hours later. A positive test involves the appearance of erythematous papules or erythematous papules with pustules at the puncture site. Patients undergoing intravenous puncture or intramuscular injection may similarly exhibit positive skin reactions.
Diagnosis and Differential Diagnosis
The internationally recognized 2014 diagnostic criteria for Behçet's disease use a weighted scoring system to evaluate individual criteria, with a total score of 4 or above confirming the diagnosis.
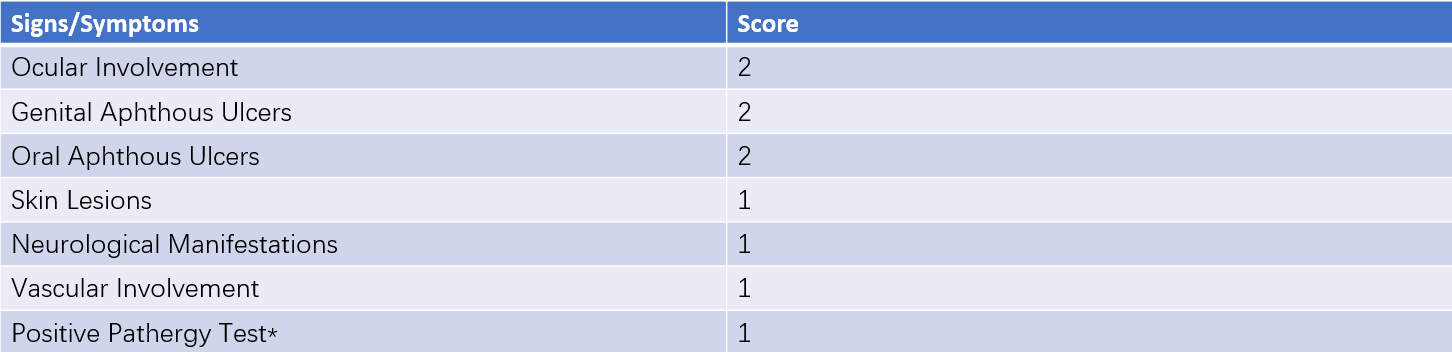
Table 1 International criteria for Behçet’s disease
Note:
Pathergy test is an optional criterion.
Oral Aphthous Ulcers: Defined as at least three confirmed occurrences of oral ulcers within one year.
Genital Aphthous Ulcers: Refers to vulvar or genital ulcers either confirmed by a physician or reported confidently by the patient.
Ocular Involvement: Includes findings such as anterior uveitis, posterior uveitis, retinal vasculitis, or vitreous cells observed under a slit-lamp examination.
Skin Lesions: Includes erythema nodosum, pseudofolliculitis, papulopustular lesions, acneiform nodules in non-adolescent individuals, and those not treated with glucocorticoids.
Due to the overlap of symptoms such as oral ulcers, arthritis, and vasculitis with other connective tissue diseases, Behçet's disease must be differentiated from conditions such as reactive arthritis, Stevens-Johnson syndrome, and systemic lupus erythematosus.
Treatment
Treatment can be categorized into symptomatic management, therapy for organ involvement and ocular inflammation, and surgical intervention.
Symptomatic Management
Different medications are selected based on individual clinical symptoms.
Topical Glucocorticoids
Glucocorticoid ointments or creams can be applied locally for patients with oral or genital ulcers.
Eye drops or eye ointments can be used to manage mild anterior uveitis effectively.
Colchicine
Colchicine is the first-line medication for preventing the recurrence of mucocutaneous lesions, particularly erythema nodosum and genital ulcers. It also shows some efficacy in managing oral ulcers.
Thalidomide
Thalidomide is effective in treating mucosal ulcers, especially oral mucosal ulcers. The recommended daily dose is 25–100 mg. However, it carries a risk of teratogenic effects such as "phocomelia," and its use is contraindicated during pregnancy.
Therapy for Organ Involvement and Ocular Inflammation
The primary medications used are glucocorticoids and immunosuppressants. Drug selection, dosage, and administration routes depend on the site and progression of the lesions.
Posterior Uveitis
Combined treatment with glucocorticoids and azathioprine, cyclosporine, interferon-alpha, or TNF-alpha inhibitors (e.g., infliximab) may be employed.
Deep Vein Thrombosis
Acute deep vein thrombosis is managed with a combination of glucocorticoids and immunosuppressants, such as azathioprine, cyclophosphamide, or cyclosporine.
Gastrointestinal Involvement
Patients with gastrointestinal lesions may benefit from glucocorticoids combined with azathioprine or TNF-alpha inhibitors.
Central Nervous System Involvement
A high-dose glucocorticoid regimen combined with immunosuppressants such as azathioprine or TNF-alpha inhibitors is recommended for cases involving the central nervous system.
Surgical Intervention
Arterial aneurysms may require interventional therapy or surgical excision based on clinical recommendations. Emergency surgical procedures may be necessary in cases of gastrointestinal complications, such as perforation, massive bleeding, or obstruction.
Prognosis
The prognosis is favorable for most patients. However, ocular involvement can lead to vision loss and, in severe cases, blindness. Gastrointestinal complications, such as ulcer bleeding, perforation, fistula formation, malabsorption, and infections, are major contributors to high mortality rates.