Gout is a form of crystalline arthritis caused by the deposition of monosodium urate crystals in the joints. Its underlying mechanism involves hyperuricemia, which results from excessive production of uric acid during purine metabolism and/or impaired uric acid excretion. The preclinical stage is characterized by asymptomatic hyperuricemia and/or urate crystal deposition, while the clinical stage manifests as recurrent acute arthritis and chronic tophaceous arthritis. Severe cases may lead to joint destruction and kidney dysfunction. Gout is often associated with comorbidities such as hyperlipidemia, hypertension, diabetes, atherosclerosis, and coronary artery disease. The prevalence of gout varies significantly worldwide depending on factors such as geographical location, ethnicity, diet, and age.
Etiology and Pathogenesis
The etiology and pathogenesis are not yet fully understood.
Formation of Hyperuricemia
Details about this can be found under the section on hyperuricemia.
Development of Gout
Hyperuricemia forms the basis for gout, with 5%–12% of hyperuricemic individuals progressing to develop gout. Acute arthritis is triggered by an inflammatory reaction to urate crystal deposition in the joints. Chronic deposition of urate crystals leads to the infiltration of neutrophils, monocytes, epithelial cells, and macrophages, forming foreign body nodules known as tophi. Based on the causes of hyperuricemia, gout can be categorized as primary, secondary, or idiopathic.
Primary gout constitutes the majority of cases and results from a combination of genetic and environmental factors. It often exhibits familial susceptibility.
Secondary gout develops as a consequence of other diseases or medications, such as glycogen storage diseases, deficiency of fructose-1-phosphate aldolase, autosomal dominant or recessive polycystic kidney disease, chronic kidney disease, or the use of certain drugs.
Clinical Manifestations
Natural Course of Gout
Gout commonly affects males over the age of 40 and postmenopausal females. The natural course includes a preclinical stage (asymptomatic hyperuricemia and monosodium urate crystal deposition) and a clinical stage (recurrent acute arthritis, intercritical periods, and chronic tophaceous arthritis).
Preclinical Stage
This stage is marked by fluctuating or persistent hyperuricemia and monosodium urate crystal deposition, which may last for several years or even a lifetime.
Acute Arthritis Stage and Intercritical Stage
Key features of this stage include the following:
- Sudden onset, most often during midnight or early morning, with severe joint pain. Within a few hours, the affected joint develops redness, swelling, heat, pain, and impaired function.
- The first metatarsophalangeal joint is the most commonly involved.
- Episodes are self-limiting and typically resolve spontaneously within two weeks.
- Hyperuricemia may accompany the episodes, although some patients exhibit normal serum uric acid levels during acute attacks.
- The presence of urate crystals in joint fluid or tophi confirms the diagnosis.
- Symptoms respond quickly to colchicine treatment.
- Fever and other systemic symptoms may be present.
The intercritical stage refers to asymptomatic periods between gout episodes.
Tophaceous Gout and Chronic Arthritis Stage
Tophi represent a characteristic clinical feature of gout. They typically occur in locations including the auricle, around joints, the olecranon, Achilles tendon, and the patellar bursa. Tophi appear as raised, yellowish-white nodules of varying sizes with thin overlying skin. Rupture may release white chalky or paste-like material. Chronic tophaceous arthritis is common in patients who have not received adequate treatment. Affected joints exhibit asymmetric, irregular swelling, pain, deformity, and functional impairment. Extensive tophus deposition within joints may result in severe bone destruction.
Renal Involvement and Comorbid Conditions
Patients with gout should be assessed for concurrent renal diseases, metabolic syndrome, and cardiovascular and cerebrovascular disorders.
Renal Involvement
Urate deposition in the urinary tract can lead to acute or chronic urate nephropathy and urolithiasis.
Acute Renal Failure
This may result from massive urate crystal deposition blocking renal tubules, renal pelvis, or ureters, leading to sudden-onset oliguria or anuria and progression to acute renal failure. This is often secondary to conditions such as malignancies undergoing chemotherapy or radiotherapy.
Chronic Gouty Nephropathy
The onset of chronic gouty nephropathy is insidious and is primarily caused by long-term deposition of monosodium urate crystals in the distal collecting ducts and renal interstitium, leading to chronic damage. Clinical manifestations include reduced urinary concentrating ability, resulting in increased nocturnal urination, low specific gravity urine, small molecular proteinuria, leukocyturia, mild hematuria, and the presence of casts. In advanced stages, patients may develop renal insufficiency accompanied by hypertension, edema, and anemia.
Uric Acid Nephrolithiasis
Uric acid nephrolithiasis may be asymptomatic or may present with symptoms such as renal colic, hematuria, difficulty urinating, hydronephrosis, pyelonephritis, or perinephritis.
Comorbidities
Metabolic Syndrome
Gout is often associated with metabolic abnormalities such as obesity, hyperlipidemia, hypertension, and impaired glucose tolerance or type 2 diabetes.
Cardiovascular Diseases
Hyperuricemia is an independent risk factor for cardiovascular diseases and contributes to their onset and progression.
Neurological Disorders
Hyperuricemia increases the risk of ischemic stroke. However, physiologic levels of serum uric acid are necessary for maintaining neurological function, and excessively low uric acid levels may be harmful to the nervous system.
Laboratory and Other Examinations
Routine Tests
Routine tests include complete blood count, urinalysis, liver and kidney function tests, blood glucose, blood lipids, erythrocyte sedimentation rate (ESR), and C-reactive protein (CRP).
Serum Uric Acid Measurement
Normal serum uric acid levels in adult males range from 208 to 416 μmol/L (3.5–7.0 mg/dL), while levels in females range from 149 to 358 μmol/L (2.5–6.0 mg/dL), although postmenopausal levels are similar to those in males. Serum uric acid levels can fluctuate significantly, so repeated measurements are recommended.
Urinary Uric Acid Measurement
Under a normal diet, the 24-hour urinary uric acid excretion is less than 800 mg, indicating reduced uric acid excretion.
Joint Fluid or Tophus Content Analysis
Polarized light microscopy reveals needle-shaped, birefringent urate crystals.
Ultrasound
Joint ultrasonography may reveal the "double contour sign" or heterogeneous echogenicities presenting as mixed hypoechoic and hyperechoic nodules.
X-Ray
Findings may include soft tissue swelling, cartilage margin destruction, irregular joint surfaces, and characteristic punched-out or moth-eaten bone erosions. Pure uric acid calculi may be radiolucent, rendering them undetectable on X-rays.
CT and MRI
CT scans can reveal high-density tophi as heterogeneous speckled lesions in affected areas. Dual-energy CT can specifically identify urate crystals and may serve as a diagnostic imaging tool while considering the potential for false positives. MRI shows low-signal, speckled lesions on T1- and T2-weighted imaging.
Diagnosis
The 2015 American College of Rheumatology (ACR) and European League Against Rheumatism (EULAR) classification criteria for gout are currently used for diagnosis.
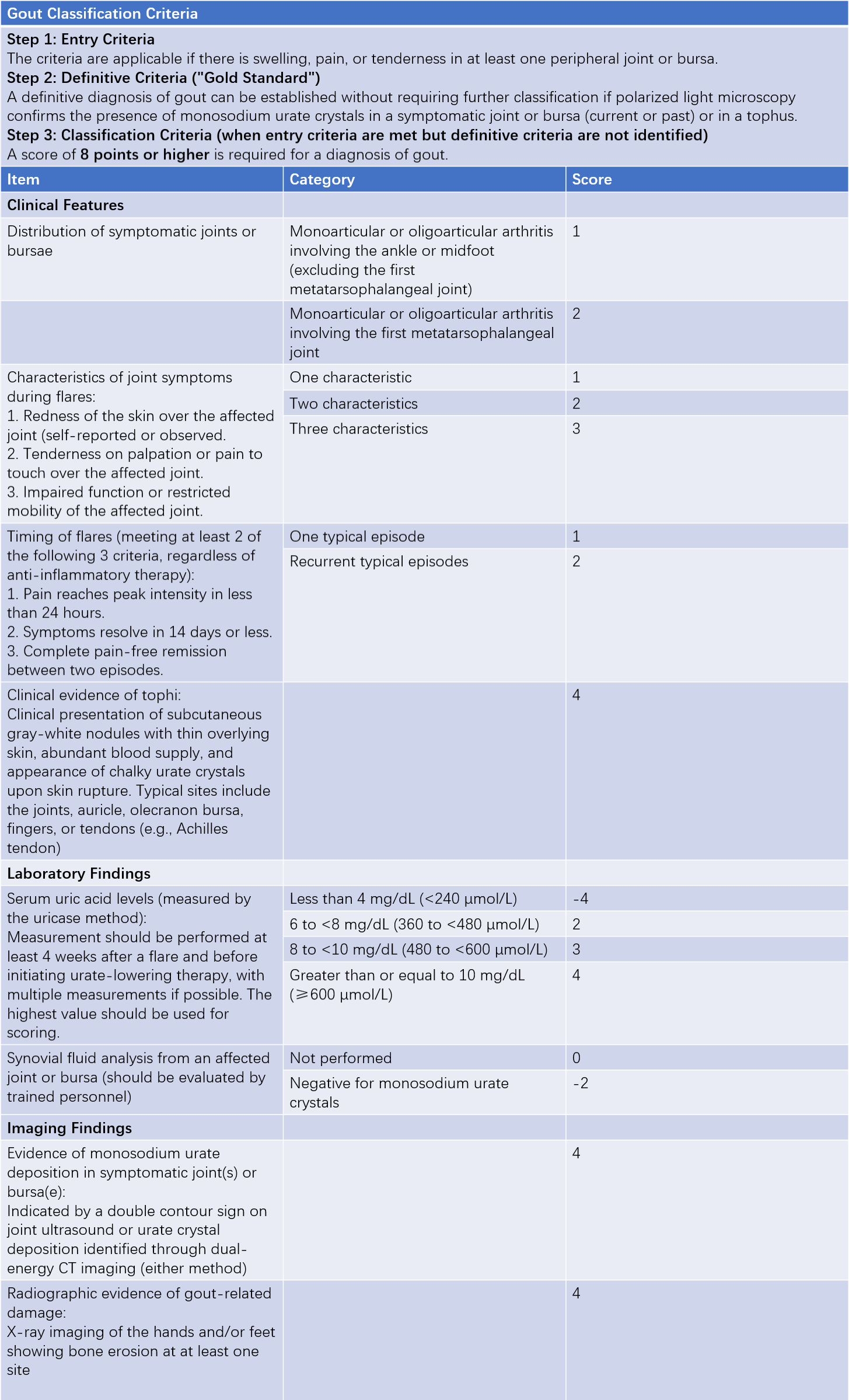
Table 1 2015 ACR/EULAR gout classification criteria
Differential Diagnosis
Gout should be differentiated from purulent arthritis, traumatic arthritis, reactive arthritis, rheumatoid arthritis, and calcium pyrophosphate deposition disease.
Prevention and Treatment
The principles of gout prevention and treatment include the following:
- Managing hyperuricemia and preventing urate deposition.
- Rapidly alleviating acute gouty arthritis flare-ups.
- Preventing the formation of uric acid calculi and protecting kidney function.
- Addressing comorbidities.
Non-Pharmacological Treatment
Patients with gout should adhere to the following principles:
- Limiting alcohol consumption.
- Reducing the intake of high-purine foods.
- Avoiding strenuous physical activity or sudden exposure to cold.
- Minimizing the consumption of fructose-rich beverages.
- Maintaining adequate hydration (at least 2,000 mL of water daily).
- Controlling weight.
- Increasing the intake of fresh vegetables.
- Following a regular diet and maintaining consistent sleep patterns.
- Engaging in regular exercise.
- Avoiding smoking.
Pharmacological Treatment
Treatment of Acute Gouty Arthritis
Colchicine, nonsteroidal anti-inflammatory drugs (NSAIDs), and corticosteroids are the first-line treatments for acute gouty arthritis and should be initiated as early as possible. Uric acid–lowering therapy is not recommended during an acute attack, although ongoing uric acid–lowering medications may be continued to avoid serum uric acid fluctuations that could prolong the attack or trigger a recurrence.
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)
NSAIDs effectively alleviate the symptoms of acute gouty arthritis. Commonly used medications include indomethacin, diclofenac, and etoricoxib. Common adverse effects include gastrointestinal ulcers and bleeding, with cardiovascular adverse events also requiring attention. Individuals with active gastrointestinal ulcers should avoid these medications, and caution is advised in those with renal impairment.
Colchicine
Low-dose colchicine (no more than 1.5 mg/day) is effective and has fewer adverse effects. Its efficacy is greater when initiated within 48 hours of symptom onset.
Glucocorticoids
Glucocorticoids are applicable in cases where NSAIDs and colchicine are ineffective or contraindicated, particularly in patients with renal insufficiency. Short-term use of moderate-dose oral glucocorticoids or intra-articular injections has shown significant efficacy in managing acute gouty arthritis.
Management During Intercritical and Chronic Phases
The target for serum uric acid in gout patients is less than 6 mg/dL (360 μmol/L) and should be maintained long-term. For patients with tophi, chronic gouty arthritis, or frequent acute gout attacks (more than two per year), the serum uric acid target is less than 5 mg/dL (300 μmol/L), but levels should not fall below 3 mg/dL (180 μmol/L). Once these conditions improve, the target can be adjusted to less than 6 mg/dL and maintained for life. Uric acid–lowering medications currently include agents that reduce uric acid production and those that promote uric acid excretion. When a single medication is insufficient, or when serum uric acid levels are markedly elevated or significant tophi formation is present, a combination therapy involving both classes of medications may be used. Other agents include alkaline drugs and uricase preparations. Preventive use of low-dose colchicine (0.5–1 mg/day) for 3–6 months during the initial stages of uric acid–lowering therapy can help reduce the risk of acute gout flares during treatment.
Uric Acid Synthesis Inhibitors
Allopurinol and febuxostat inhibit xanthine oxidase activity, reducing uric acid synthesis.
The starting dose of allopurinol is 50–100 mg/day, which can be gradually increased over four weeks to a maximum dose of 600 mg/day. Adverse reactions include gastrointestinal discomfort, rash, drug-induced fever, and liver function abnormalities. Lower starting doses are recommended in patients with renal impairment, and individuals with an HLA-B*5801 gene variation should avoid using allopurinol.
Febuxostat is initiated at 20–40 mg/day, with a maximum dose of 80 mg/day. Dose adjustment is generally unnecessary in mild-to-moderate renal impairment. Adverse effects include liver function abnormalities, gastrointestinal reactions, and cardiovascular events; caution is advised in patients with coexisting coronary artery disease.
Medications That Promote Uric Acid Excretion
Benzbromarone inhibits the reabsorption of urate by the proximal renal tubular urate transporters, thereby increasing uric acid excretion. The initial dose is 25–50 mg/day, with a maximum dose of 100 mg/day. During treatment, patients are advised to increase water intake and alkalinize their urine. Adverse reactions include rash, gastrointestinal symptoms, liver function abnormalities, and renal colic. Benzbromarone is contraindicated in those with an estimated glomerular filtration rate (eGFR) of less than 20 mL/min or a history of urinary stones.
Other Uric Acid–Lowering Medications
Uricase preparations such as rasburicase and pegloticase convert uric acid into allantoin, which is excreted via the kidneys. These are not yet indicated for routine use and are not considered first-line therapies.
Treatment of Comorbidities
Gout is often associated with one or more components of metabolic syndrome, including hypertension, hyperlipidemia, obesity, and type 2 diabetes, all of which should receive appropriate treatment. For patients with hypertension, medications such as losartan or amlodipine are preferred, while lipid-lowering agents such as fenofibrate or atorvastatin are recommended. In gout patients with chronic kidney disease, drugs with minimal renal impact should be selected.
Surgical Treatment
Surgical options may include the removal of tophi or corrective procedures for damaged joints in cases where necessary.
Prognosis
The prognosis for gout is favorable when early and standardized treatment is initiated. However, without proper treatment, joint damage, diminished quality of life, and reduced life expectancy may occur.