Rheumatic fever is a delayed inflammatory complication caused by pathogenic streptococcal infections. Recurrent episodes often leave varying degrees of cardiac damage, leading to rheumatic heart disease. It is most common during the rainy seasons of winter and spring, particularly in impoverished and underdeveloped regions. The condition primarily affects children and adolescents aged 5–15 years. Although the global incidence has significantly declined, eradicating the disease remains a significant challenge.
Pathogenesis
Streptococcal pharyngeal infection is an essential condition for the development of rheumatic fever, with rheumatogenic streptococci primarily belonging to groups A–C, particularly group A. The exact pathogenesis remains unclear, but possible mechanisms include the following: Streptococcal components that share similarity with self-antigens may activate autoreactive B and T cells through a molecular mimicry mechanism, leading to the formation of immune complexes and subsequent tissue damage. Epitope spreading may further exacerbate tissue injury.
Genetic susceptibility is associated with disease onset, with the immunoglobulin heavy chain locus and human leukocyte antigen (HLA) class II region identified as susceptibility loci. Environmental factors also play a significant role, as overcrowded living conditions and routine antibiotic use for acute pharyngitis contribute to the high incidence of the disease.
Pathological Anatomy
Rheumatic fever can result in damage to various tissues. The characteristic pathological feature is the "Aschoff body," formed by fibrinoid degeneration involving connective tissue, lymphocyte infiltration, and proliferation of abnormal histiocytes.
Cardiac valves may show thickening, calcification, and distortion, with crescent-shaped edges and T-cell infiltration. The mitral valve is the most commonly affected, followed by the aortic valve.
Clinical Manifestations
Symptoms
The disease usually presents acutely, often occurring 1–5 weeks after streptococcal pharyngitis (or streptococcal pyoderma in tropical regions). Key manifestations include arthritis, carditis, chorea, subcutaneous nodules, and erythema marginatum, which may appear individually or in combination. Approximately 70%–75% of patients exhibit acute fever with arthritis, often accompanied by carditis.
Arthritis
The most common symptom, characterized by acute, polyarticular, migratory, and non-deforming arthritis. The knees, ankles, elbows, and wrists are most frequently affected. Symptoms typically last for 1–7 days.
Carditis
Classic cases involve pancarditis, affecting the pericardium, epicardium, myocardium, and endocardium, with the mitral and aortic valves most frequently involved. Cardiac manifestations typically appear within 3 weeks after streptococcal infection. Severe or recurrent cases may lead to rheumatic heart disease and heart failure.
Chorea
This usually appears 1–8 months after streptococcal infection and may present in isolation. It is more common in girls and typically resolves completely within 6 weeks, though it may recur during pregnancy or with the use of oral contraceptives.
Erythema Marginatum
Non-itchy lesions become more apparent with heat and resolve within hours or 1–2 days.
Subcutaneous Nodules
These present as hardened, painless nodules located on the extensor sides of joints. They are often symmetrically distributed, averaging 3–4 in number, and persist for 1–several weeks.
Other Symptoms
Additional manifestations include fever, excessive sweating, and abdominal pain.
Signs
Observable signs include erythema marginatum and subcutaneous nodules. Sinus tachycardia represents an early indication of carditis. Cardiac valve involvement may present with corresponding physical signs.
Auxiliary Tests
Laboratory Tests
Indicators of streptococcal infection are detailed in Table 1.
During the acute phase, 80% of patients present with elevated ESR and CRP levels.
Synovial fluid analysis typically shows sterile inflammatory fluid.
Additional Examinations
Echocardiography/Doppler ultrasound and resting electrocardiography are recommended for all suspected cases of rheumatic fever.
Diagnosis
The diagnosis can be made based on the Jones Diagnostic Criteria revised by the American Heart Association in 2015.
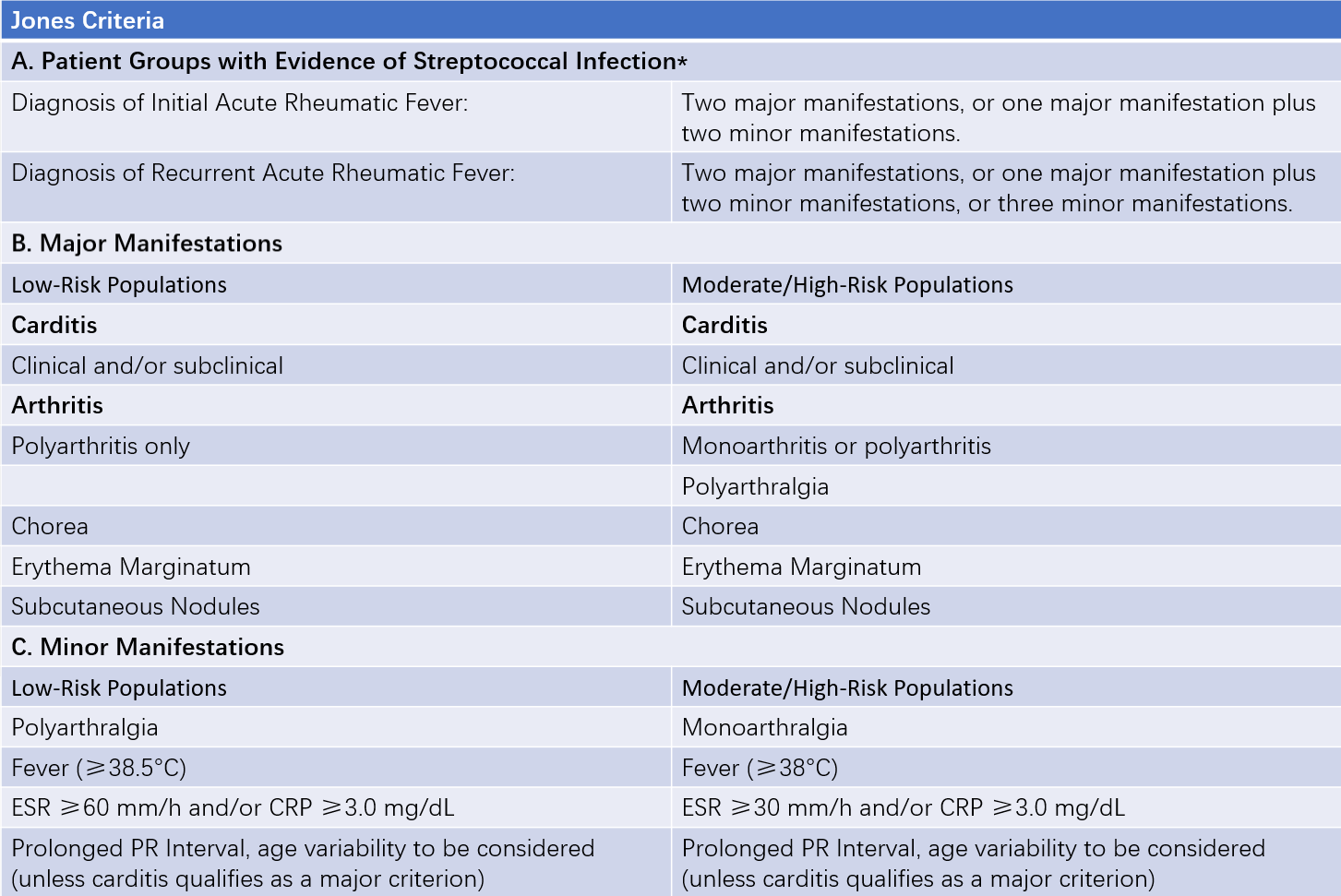
Table 1 2015 revised Jones criteria by the American heart association
Notes:
*Evidence of streptococcal infection refers to:
Positive pharyngeal swab culture for Group A β-hemolytic streptococci.
Positive rapid streptococcal antigen test.
Elevated or rising anti-streptolysin O (ASO) titers or anti-deoxyribonuclease B antibodies, either of which may be positive.
If streptococcal infection is suspected, sampling may be repeated after two weeks.
Manifestations of arthritis and arthralgia, as well as carditis and prolonged PR interval, qualify as either a major or minor criterion, but not both simultaneously.
Differential Diagnosis
The causes of polyarthritis need to be broadly differentiated, including infections, post-infectious immune responses, other rheumatic diseases, and malignancies.
Treatment
The treatment focuses on four primary objectives: eradication of pathogenic streptococcal infection with antibiotics; rapid management of clinical symptoms; control of complications and comorbidities such as heart failure and chorea; and prevention of recurrent infections.
The treatment plan should adhere to an individualized approach. Eradication of streptococci aims to prevent recurrences, with penicillin as the first-line choice. Nonsteroidal anti-inflammatory drugs are preferred for managing arthritis.
Prognosis
Approximately 70% of patients achieve recovery within 2–3 months. Individuals with acute cardiac involvement who do not receive timely and appropriate treatment may develop rheumatic heart disease, which is the most common acquired valvular defect.
Prevention
Primary Prevention
Early diagnosis and antibiotic treatment of streptococcal infections are essential to prevent the development of rheumatic fever.
Secondary Prevention
Continuous use of effective antibiotics in individuals with a clear clinical history or confirmed rheumatic heart disease is crucial to prevent recurrence and mitigate further cardiac damage.